Today, I review some surprising new data on a crucial aspect of the drug channel: how employer-sponsored health plans access the billions of dollars in manufacturer rebates that are negotiated by their PBMs.
As Barbie learned, the real world isn’t what you thought it was. Only about 60% of employers report that their PBM passes through all rebates on traditional and specialty drugs. What's more, one-third of employers choose spread pricing for their pharmacy network.
These data seem to contradict public statements by PBM executives, while also undermining the purpose of legislation that mandates rebate pass-through to plan sponsors. Notably, most of the proposed legislation fails to mandate pass-through to the patients whose prescriptions generated the rebates.
Read on for the details. Although when you find out that PBM reform isn’t about horses, you may lose interest.
LET’S GO PARTY
To evaluate employer-PBM relationships, we rely on the 2023 Trends in Drug Benefit Design Report and the 2023 Trends in Specialty Drug Benefits Report. Both of these valuable new reports come from Pharmaceutical Strategies Group (PSG), and are free with registration. As always, I encourage you to review the original source material for yourself. For historical perspective, we use a predecessor survey conducted in 2014 by the Pharmacy Benefit Management Institute (PBMI), which PSG acquired in 2020.
The PSG survey collected data from employers, not from PBMs. The 2023 drug benefits report includes responses from 113 employer-sponsored plans. The 2023 specialty drug benefits report includes responses from 124 employer-sponsored plans.
Only a subset of the employers answered questions about rebate agreements. Consequently, the sample sizes were fairly small. However, as far as I know, these reports provide us with the only available public information about the nature of the relationships between PBMs and their employer-based health plan clients. Note that PSG provided me with some additional data, so the figures below may not correspond precisely with the published reports.
OPENING A PORTAL TO THE REAL WORLD
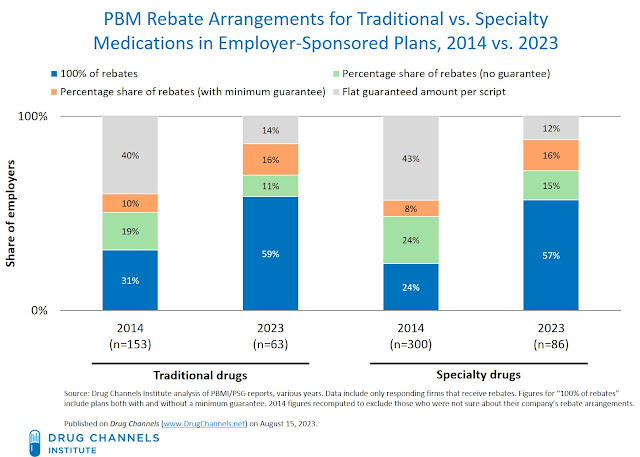
The chart below summarizes employers’ reported rebate relationships for traditional drugs in 2014 vs. 2023.
[Click to Enlarge]
Observations on these data:
- Employers have moved away from flat guaranteed per-script rebates. In 2014, a flat guaranteed per-script rebate amount (grey bars above) was the most common form of rebate contracting for both small and large employers. By 2023, most employers are instead opting for full rebate pass-through (blue bars) or receiving a share of the rebates (green and orange bars).
- Most—but not all—employers report receiving 100% pass-through of the rebates negotiated by their PBM. For 2023, a majority of small and large employers report receiving 100% of rebates for traditional drugs. The figures for “100% of rebates” include plans both with and without a minimum guarantee. Adoption of full rebate pass-through has increased significantly over the past nine years. (See the blue bars in the chart above.) For employers that chose not to receive full rebate pass-through, the value of the rebates were presumably factored into the prescription prices that the PBM charged the employer.
- The employer-reported figures are much lower than the pass-through percentages described by PBMs. For both traditional and specialty drugs, slightly less than 60% of employers report receiving 100% of rebates. There was one notable difference in the 100% pass-through rebate responses between large and small employers. For traditional drugs, 50% of larger employers—those with 5,000 or more beneficiaries—report receiving 100% of rebates with a minimum guarantee, while only 30% of smaller employers received a minimum guarantee. (See Figure 54 in the full report.)
The 100% pass-through figures shown above are lower than what PBMs have stated. Let’s go all the way to the top and consider these statements from a May Congressional hearing:
- Adam Kautzner, president of Express Scripts, testified that the company “passed through over 95% of rebates it collected for its clients in 2022.”
- David Joyner, executive vice president and president of Pharmacy Services for CVS Health, testified: "[W]e pass more than 98% of all rebates back to our clients.”
- The survey figures reflect the share of employers, which could differ from the share of rebate dollars.
- There could be undisclosed client differences. For government programs, PBMs pass through the full value of rebates to Medicare Part D plans and the state and federal payers for Medicaid. But as far as I know, PBMs have not reported rebate pass-through rates that are specific to employer-sponsored plans.
- The employer respondents to the PSG surveys may have a different definition of “rebates” compared with the PBM executives.
- The PSG samples were too small to be representative of the entire employer population.
That should trouble anyone concerned that legislation will mandate a rebate model that many employers seem not to choose. For example, the Pharmacy Benefit Manager Reform Act (S.1339) has a provision that requires “full rebate pass-through to plan or health insurance issuer.” That’s one reason why PBMs find this idea scarier than your feet going flat.
What's more, one-third of employers compensate their PBMs using spread pricing in their pharmacy networks. (See Figure 55 in the Trends in Drug Benefit Design Report.) This means that legislation banning spread pricing seems to go against the revealed preferences of plan sponsors. Paging Legislative Aide Barbie!
Another reality: PBMs earn a declining share of their profits from retained rebates and retail network spreads. DCI estimates that the large PBMs now generate a majority of their profits from pharmacy buy-sell dispensing spreads along with profits from the 340B Drug Pricing Program, copay maximizers, group purchasing organizations, and other manufacturer services. (For our deconstruction of the major sources of PBM profits, see Section 11.2.3. of our our 2023 Economic Report on U.S. Pharmacies and Pharmacy Benefit Managers.) Does the label "long-term long-distance low-commitment casual vendor" mean nothing to employers?
IN THE PINK
Rebates can reduce a third-party payer’s net prescription costs as funds flow through the channel. Plan sponsors and PBMs argue that “rebates lower costs for patients.” But that’s only partially accurate—and why current pass-through legislation falls short for patients.
The available evidence suggests that employers typically use rebates to offset overall healthcare costs and reduce general premiums, rather than reduce the out-of-pocket prices paid by the patients whose prescriptions generated the rebate funds. (See Section 9.1.1. of our pharmacy/PBM report.) That’s not closer to fine.
Consider The 2023 Milliman Medical Index, which estimated that pharmacy benefit drug rebates reduced total per-person pharmacy benefit costs by $439 (-27%). This analysis found that most (70%) of the value of these rebates was applied to the employer’s premium contribution, while the remainder (30%) was applied to the average employee’s premium contribution. None of the rebate value was applied to reducing out-of-pocket costs for prescriptions.
As Milliman noted: “In most employer-sponsored PPO plans today, rebates do not affect an employee’s out-of-pocket costs.” Even Weird Barbie would be troubled by this statement.
As a result, people with chronic, complex diseases generate billions in rebate dollars, which are then used to lower the premiums of healthier beneficiaries. This is the reverse insurance problem. As former FDA commissioner Scott Gottlieb noted: “sick people aren’t supposed to be subsidizing the healthy.”
Over time, it will become harder to put this notion back into its box. I suspect that PBM reform will eventually turn to how commercial plan sponsors' rebate strategies affect patients’ out-of-pocket prescription costs. Will that be Kenough?


No comments:
Post a Comment