For 2024:
- 94% of stand-alone Medicare Part D prescription drug plans (PDP) will have a preferred network.
- 51% of Medicare Advantage prescription drug (MA-PD) plans will have a preferred network.
The 2024 data provide early evidence of a shrinking PDP market. Chalk it up to yet another unintended consequence of the Inflation Reduction Act of 2022 (IRA), which will make PDPs less economically viable and drive even more seniors into Medicare Advantage plans.
D IS FOR DATA
A preferred network gives consumers a choice of pharmacy while providing financial incentives to use the pharmacies that offer the payer lower costs or greater control. A consumer with a preferred network benefit design retains the option of using any pharmacy in the network. However, the consumer’s out-of-pocket expenses will be higher at a non-preferred pharmacy.
Preferred network models have grown rapidly within the Medicare Part D program, where CMS calls them preferred cost sharing networks. CMS calls the pharmacies in such networks preferred cost sharing pharmacies.
According to federal regulations, preferred pharmacies in Part D must offer “covered Part D drugs at negotiated prices to Part D enrollees at lower levels of cost sharing than apply at a non-preferred pharmacy under its pharmacy network contract.” (source) Beneficiaries who qualify for the Low-Income Subsidy (LIS) face low out-of-pocket drug costs regardless of a pharmacy’s preferred status.
To identify the 2024 Part D preferred cost sharing pharmacy networks, we used the 2024 Plan Finder Data (September 29, 2023) and the 2024 Landscape Source Files (October 5, 2023) for PDPs and MA plans.
Our analysis of stand-alone PDPs eliminated the following plans from the sample:
- Employer-sponsored plans
- Plans from U.S. territories and possessions (American Samoa, Guam, Northern Mariana Islands, Puerto Rico, Virgin Islands)
- Employer/union-only group plans (contracts with "800 series" plan IDs)
D-LIMITING
Our final PDP sample included 60 PDPs, which will operate 709 regional PDPs:
- Fourteen plans are being offered in all 34 regions, for a total of 476 PDPs (=14*34).
- Four plans are operating in 33 regions, one plan is operating in 18 regions, and one plan is operating in 16 regions. These six plans account for a further 166 regional PDPs.
- The remaining 40 plans are operating in eight or fewer regions and account for 67 PDPs. Many of these plans are state-level Blue Cross Blue Shield plans.
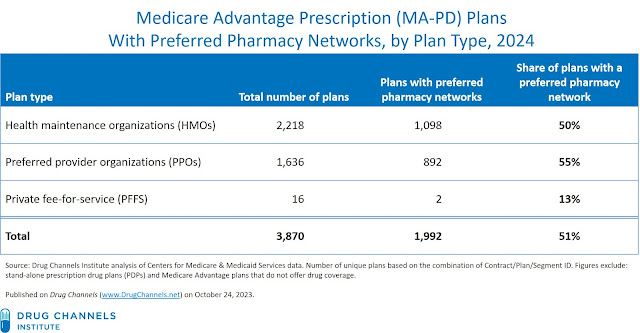
- Health maintenance organizations (HMOs): 2,218 local plans
- Preferred provider organizations (PPOs): 1,636 local plans and 32 regional plans
- Private fee-for-service (PFFS) plans: 16 plans
PART D-CLINE
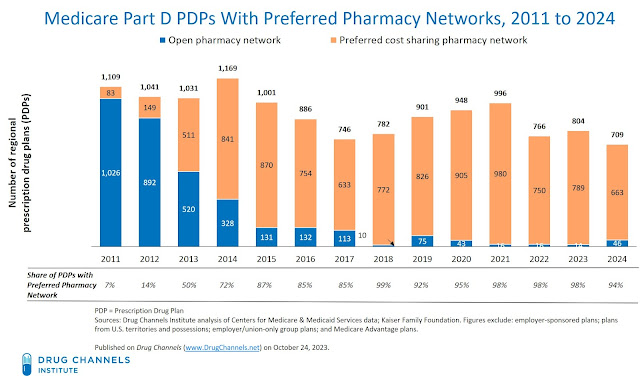
The chart below shows the growth of preferred networks in stand-alone prescription drug plans. In 2011, only 7% of total regional PDPs had a preferred network. For 2024, 94% of Medicare Part D regional prescription drug plans (PDP) will have a preferred network. Penetration declined slightly from previous years because one of Humana’s plans switched to an open network. (Details below.)
[Click to Enlarge]
Since 2018, the share of plans with a preferred network has remained above 90%. During this period, however, the total number of plans has fluctuated. For 2022, the number of stand-alone PDPs dropped by -23%, from 966 to 766 plans. As we discussed in a previous analysis, this drop reflected consolidation among plan sponsors. For 2023, the number of plans rebounded, to 804 plans. The increase was due almost entirely to the Mutual of Omaha’s introduction of a third plan option (discussed below).
For 2024, the number of PDPs will be lower than at any time since at least 2011.
MA-PDs are much less likely to offer plans with preferred pharmacy networks. Overall, only 51% of these plans will have preferred networks, which is comparable to the previous year’s share. The prevalence of preferred pharmacy networks will vary by plan type:
[Click to Enlarge]
Part D enrollment in MA-PD plans has increased over time, while enrollment in stand-alone PDPs has decreased in recent years. (source) I suspect more open pharmacy networks are contributing to this trend.
D IS FOR DOMINANT
Here are the 2024 highlights from the seven major companies with national stand-alone PDPs. These companies account for 642 (91%) of the total 709 PDPs. Only one of these companies’ plans will have an open retail network. All of the other plans will have preferred cost sharing networks.
- Aetna Medicare will offer the two legacy CVS Health SilverScript Choice and Plus plans as well as a new SilverScript SmartSaver plan, which will replace the SilverScript SmartRx plan that was launched in 2021. Recall that CVS Health’s Part D business is now integrated with Aetna and reported within the company’s Health Care Benefits segment.
- Cigna will offer three plans: Extra, Saver, and Secure. The Saver plan was introduced for 2023 and includes low premiums, low copays, and an emphasis on generic drug savings. Note that Express Scripts no longer offers its own plans separately from Cigna.
- Clear Spring Health entered the market in 2020 and will offer only one plan with a preferred network: Clear Spring Health Value Rx. It has discontinued the Clear Spring Health Premier Rx plan. Clear Spring Health is part of the Group One Thousand One insurance company.
- Humana will offer the three plans that it has offered since 2020—Basic Rx, Premier Rx Plan, and the Humana Walmart Value Rx Plan. The Humana Basic Rx plan switched from an open network to a preferred retail network for 2021, but will switch back to an open network for 2024.
- Mutual of Omaha Rx will offer its Rx Essential (launched for 2023), Rx Plus, and Rx Premier plans. Mutual of Omaha launched its plans for the 2019 plan year and are offered through Omaha Health Insurance Company, a Mutual of Omaha affiliate company.
- UnitedHealthcare will offer three AARP-branded plans as well as a co-branded AARP MedicareRx Walgreens plan. Two of these plans—the AARP Medicare Rx Saver from UHC and the AARP Medicare Rx Basic from UHC—will be offered in only about half of the country’s regions. The Rx Basic plan is new for 2024.
- WellCare, which is now part of Centene, will offer three plans in 2024: Wellcare Classic; Wellcare Value Script; and Wellcare Medicare Rx Value Plus. All three plans have been available since 2020. In 2022, WellCare stopped offering the three plans—Rx Saver, Rx Select, and Rx Value Plus—that it had acquired as part of the Aetna-CVS Health merger.
For more on the economics and strategies of narrow networks, see Chapter 7 of our Economic Report on U.S. Pharmacies and Pharmacy Benefit Managers.
D-STABILIZING?
The IRA has scrambled the economics of Part D. Avalere estimates that 2024 MA-PD bids increased by 63%, from $31 for 2023 to $50 for 2024. PDP bids more than doubled, from $38 for 2023 to $78 for 2024.
What's more, premiums for standalone PDPs will increase by 33%. That's greater than the advertised 6% growth cap, due to a technical difference between the base beneficiary premium and individual plan premiums.
After 2025, look for many plans to flee the PDP market. Looks like the vertically integrated organizations that dominate U.S. healthcare will win again from major healthcare legislation. Good news for their shareholders, but perhaps not for the U.S. taxpayers.


No comments:
Post a Comment