- My $0.02 on the Humira price war—and the role of cost-plus pharmacy pricing
- Fresh evidence that formulary exclusions hurt patients
- Disturbing oncology drug benefit management
P.S. Join my more than 42,000 LinkedIn followers for daily links to neat stuff. You can also find my daily posts at @DrugChannels on Twitter, where I have more than 16,500 followers. (I recommend that you follow me on LinkedIn, because the quality of comments and engagement is much higher than they are on Twitter.)
Coherus Announces Industry-Wide Lowest List Price for Adalimumab Biosimilar YUSIMRY™ (adalimumab-aqvh) Launching in July 2023, Coherus BioSciences
I’ve been warning about the coming Humira price war for some time.
This month, Coherus Bioscience announced a bold Humira #biosimilar price war and a novel partnership with the Mark Cuban Cost Plus Drug Company (MCCPDC).
Coherus will set the wholesale acquisition cost (WAC) for YUSIMRY, its non-interchangeable, low concentration Humira biosimilar, at $995. That’s an 85% discount to Humira’s list price. MCCPDC will sell YUSIMRY for only $569 plus shipping.
I’m certainly not naïve. There are significant barriers to widespread adoption of a low-WAC product, including Humira’s rebate wall, PBM formulary practices, physician and patient concerns about switching to biosimilars, barriers at retail and wholesale channels, patient out-of-pocket costs, and more
Despite these challenges, I believe that the large PBMs will rapidly lose control of this market. If you attended my March 2023 video webinar, you may recall my discussion of how cost-plus pharmacy pricing could impact highly-rebated drugs, the big three PBMs’ profit models, and plan sponsor economics.
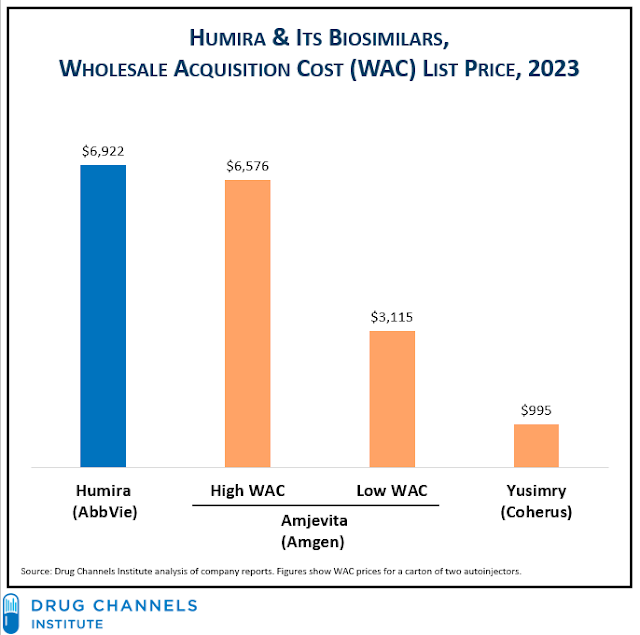
Consider the ways in which aggressive biosimilar pricing strategies could disrupt the economics of copay support. (I discussed this topic during last week's video webinar.) The chart below compares the WAC list prices of Humira to the announced prices of two biosimilars. YUSIMRY’s low price leaves little room for patient copay support. But it also prevents non-patients—plans, PBMs, and vendors—from absorbing any of that support via copay accumulators, maximizers, and alternative funding programs.
As far as I know, SmithRx will be the first PBM to offer the YUSIMRY biosimilar in partnership with Mark Cuban Cost Plus Drug Company. SmithRx is a small PBM that focuses on midsize companies with fewer than 5,000 employees.
Are plans paying attention as the gross-to-net bubble pops?
This month, Coherus Bioscience announced a bold Humira #biosimilar price war and a novel partnership with the Mark Cuban Cost Plus Drug Company (MCCPDC).
Coherus will set the wholesale acquisition cost (WAC) for YUSIMRY, its non-interchangeable, low concentration Humira biosimilar, at $995. That’s an 85% discount to Humira’s list price. MCCPDC will sell YUSIMRY for only $569 plus shipping.
I’m certainly not naïve. There are significant barriers to widespread adoption of a low-WAC product, including Humira’s rebate wall, PBM formulary practices, physician and patient concerns about switching to biosimilars, barriers at retail and wholesale channels, patient out-of-pocket costs, and more
Despite these challenges, I believe that the large PBMs will rapidly lose control of this market. If you attended my March 2023 video webinar, you may recall my discussion of how cost-plus pharmacy pricing could impact highly-rebated drugs, the big three PBMs’ profit models, and plan sponsor economics.
Consider the ways in which aggressive biosimilar pricing strategies could disrupt the economics of copay support. (I discussed this topic during last week's video webinar.) The chart below compares the WAC list prices of Humira to the announced prices of two biosimilars. YUSIMRY’s low price leaves little room for patient copay support. But it also prevents non-patients—plans, PBMs, and vendors—from absorbing any of that support via copay accumulators, maximizers, and alternative funding programs.
[Click to Enlarge]
As far as I know, SmithRx will be the first PBM to offer the YUSIMRY biosimilar in partnership with Mark Cuban Cost Plus Drug Company. SmithRx is a small PBM that focuses on midsize companies with fewer than 5,000 employees.
Are plans paying attention as the gross-to-net bubble pops?
Assessing the impact of formulary exclusion on healthcare costs and outcomes for patients on therapy for certain chronic conditions, Xcenda
In The Big Three PBMs’ 2023 Formulary Exclusions: Observations on Insulin, Humira, and Biosimilars, I lamented the lack of research on how exclusions affect physicians’ prescribing decisions, patients’ ability to access therapies, and clinical outcomes.
That’s why I’m happy to see that Xcenda has studied these issues—but disappointed in what it uncovered.
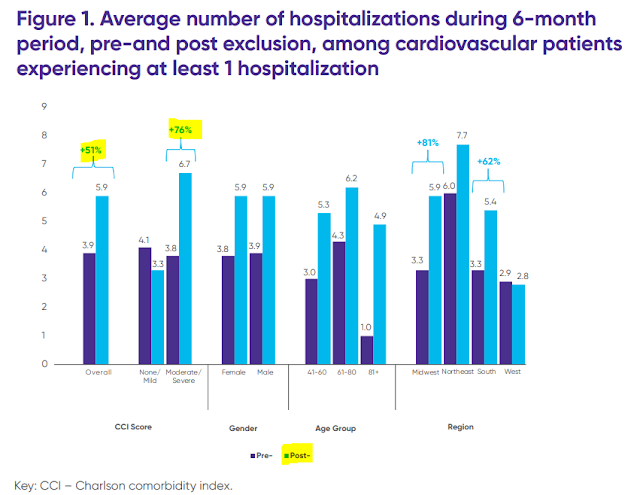
Using a case study approach, Xcenda found that formulary exclusion increases hospitalizations and emergency department visits for patients with chronic illnesses who are stable on drug therapy. The patients also incurred higher out-of-pocket costs. The chart below highlights some of the data on cardiovascular patients.
I'm troubled that exclusions have become so common—and makes me wonder the extent to which plan sponsors are providing a “benefit” that really isn't.
That’s why I’m happy to see that Xcenda has studied these issues—but disappointed in what it uncovered.
Using a case study approach, Xcenda found that formulary exclusion increases hospitalizations and emergency department visits for patients with chronic illnesses who are stable on drug therapy. The patients also incurred higher out-of-pocket costs. The chart below highlights some of the data on cardiovascular patients.
[Click to Enlarge]
I'm troubled that exclusions have become so common—and makes me wonder the extent to which plan sponsors are providing a “benefit” that really isn't.
Expanding Considerations in Oncology Access, IQVIA
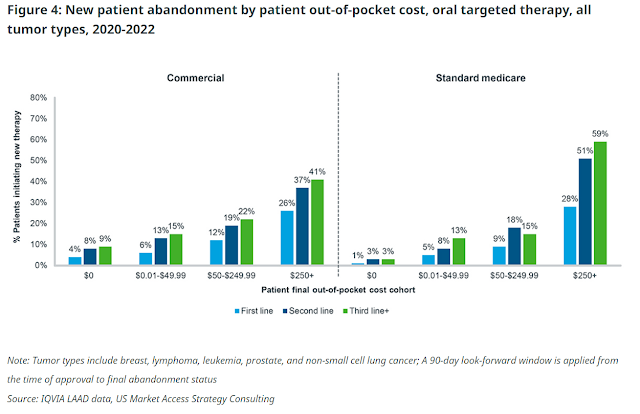
As Keanu Reeves would say: Whoa. IQVIA found stunning abandonment rates for cancer drugs—even when out-of-pocket cost is very low (or even $0). This is a benefit design problem, not a “high drug price” issue. Why should cancer patients have any "skin in the game?"
The report also includes some startling data on insurers’ prior authorization practices. For instance, insurers initially reject new oral targeted therapies for about 90% of commercial cancer patients and about 75% of Medicare patients. (See Figure 1 in the report.)
Kudos to IQVIA for providing another valuable, fact-based study of real-world benefit designs.
[Click to Enlarge]
The report also includes some startling data on insurers’ prior authorization practices. For instance, insurers initially reject new oral targeted therapies for about 90% of commercial cancer patients and about 75% of Medicare patients. (See Figure 1 in the report.)
Kudos to IQVIA for providing another valuable, fact-based study of real-world benefit designs.
The Biggest Misconceptions about American Health Care, Kite & Key Media
Here's a fantastic video explainer about why no one can explain the U.S. #healthcare system. Also, pretty funny. Highly recommended! 👍👍


No comments:
Post a Comment