Jane and Susan discuss the mechanism and benefits of warranties in the realm of value-based contracts.
To learn more about payer-pharma warranty contracts and whether these agreements can solve issues that limit the utility of more traditional value-based contracts, sign up for Real Endpoints’ free June 9 webinar: Putting Innovative Contracts Under Warranty.
Read on for Jane’s and Susan’s insights.
It’s Time to Put Innovative Contracts Under Warranty
By Jane Barlow, Chief Clinical Officer, and Susan Raiola, President, Real Endpoints LLC
Warranties are a category of value-based agreement that can be structured to be both more patient-centric and more payer friendly than many traditional value-based contracts. At the same time, they mitigate some of a biopharma’s key concerns around Medicaid Best Price, including the risk that a single, significant rebate will be passed on to every Medicaid payer.
To date, the best public example of a warranty is the so-called Pfizer Pledge for the lung cancer drug Xalkori. As part of the pledge, both patients and payers could get back 100% of their drug costs if Xalkori fails to work within the first three months. But that 100% refund won’t trigger impossibly large Medicaid rebates via the Medicaid Best Price rule. (Under that statue, Medicaid receives the better of an automatic rebate, usually 23.1%, or the best price available for the drug, which in this case could be $0.)
The reason? Pfizer isn’t paying the rebate: instead, it’s bought an insurance policy from AIG, which will pay any liabilities. Pfizer’s “best price” is merely the cost of the drug minus the risk premium, per the interpretation of the Centers for Medicare and Medicaid Services.
Stakeholders like the idea. Payers get a mechanism to recoup 100% of a drug’s cost if Xalkori doesn’t work—something that’s increasingly attractive as the number of high-cost specialty products balloons. Because there’s a dedicated third party to track and validate patient outcomes, the administrative hurdles for payers (and manufacturers) are lower too. For patients, a warranty reduces the economic burden if there is no clinical benefit, at least partly addressing the larger issue of high out-of-pocket costs.
MIND THE COSTS
But these advantages have costs. The intermediary administering and paying the warranty charges an administration fee to manage the data and adjudicate claims. This entity also charges a risk premium determined by the overall uncertainty of the drug’s future performance and the value to be paid out if the medicine underperforms. Finally, as with other kinds of insurance products, the third party needs to earn a profit for taking on and managing the risk. Depending on the population being treated and the clinical uncertainty of the drug’s performance, the sum of these costs can be significant.
Stakeholder effort shouldn’t be underestimated either. The documentation supporting a warranty claim can require significant effort from both patients and providers. Although tech-enabled solutions to simplify the data-gathering process exist, the obstacles can be discouraging for patients and caregivers managing a devastating illness. And time-strapped physicians, who receive no remuneration for the attestations they’re required to submit, may bypass warrantied drugs in favor of products with similar clinical efficacy. Payers, meanwhile, might prefer to eschew the patient portion of a warranty deal (which isn’t a mandatory feature) and/or focus on endpoints adjudicated with medical or pharmacy claims to which they already have access.
LIVING UP TO THE PROMISE
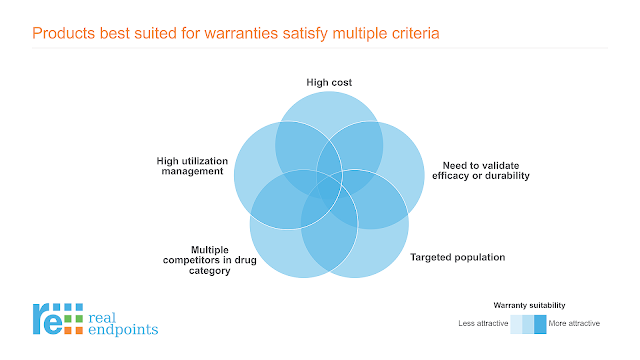
Because of the potential costs to administer a warranty through a third-party, this innovative structure is best suited for access-challenged, high-cost products that meet several additional criteria, including:
- Efficacy or durability isn’t fully locked down;
- There are few well-proven advantages over the competition;
- At least two or three other therapeutic options physicians and patients could choose.
Warranties can also work for certain cancer drugs—particularly add-ons in diseases with multiple therapeutic approaches using different mechanisms of action. They may even provide good options for less expensive but still costly specialty medicines in more prevalent disease indications where a warranty with an unusually large rebate might convince a payer to loosen its utilization management or even grant some kind of preferred access.
ANOTHER IMPORTANT TOOL IN THE TOOLBOX
Warranties won’t magically solve the access issue. And some products will fit better than others. But to accelerate the use of potentially transformative therapies, biopharma companies must actively explore this potentially important tool in the value-based movement. To learn which products are best fits for warranties and how to operationalize them, sign up for our free June 9 webinar: Putting Innovative Contracts Under Warranty.
Sponsored guest posts are bylined articles that are screened by Drug Channels to ensure a topical relevance to our exclusive audience. These posts do not necessarily reflect our opinions and should not be considered endorsements. To find out how you can publish a guest post on Drug Channels, please contact Paula Fein (paula@DrugChannels.net).



No comments:
Post a Comment