Divya highlights new GoodRx research on the out-of-pocket cost gap between brand-name and generic prescriptions. She discusses the challenges that providers face when having real-time discussions with patients about out-of-pocket costs. Divya then explains how GoodRx partners with pharmaceutical companies to improve cost transparency and communication between patients and providers.
Click here to learn more about how GoodRx helps brand teams engage providers in specific specialties.
Read on for Divya’s insights.
Improving Out-of-Pocket Cost Transparency For Physicians
By Divya Iyer, VP, Strategy & Business Development, Pharma Manufacturer Solutions, GoodRx
In the last year, more than 825,000 healthcare providers across all specialties have used the GoodRx platform for information and tools related to health conditions, generic and branded medications, and affordability and adherence support for their patients. In addition to collecting and analyzing real-world data from our platform and other sources, GoodRx researchers conduct formal studies with providers and patients on a regular basis.
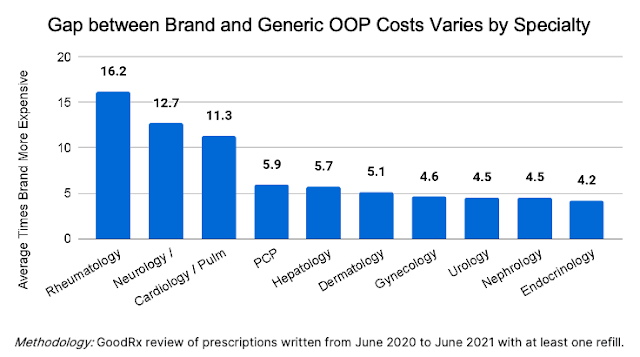
Recent insights from an analysis of patient drug costs across specialties shows interesting disparities in cost of branded versus generic medicines. Average out-of-pocket (OOP) costs for branded prescriptions are higher than for comparable generics in the same category, but the factor by which they are more expensive varies across specialties (see Figure 1).
For example, the OOP cost gap in rheumatology, neurology, and cardiology/pulmonology is much wider than in other specialties. This insight may provide opportunities for pharma manufacturers to look more closely at the specialties aligned with their portfolios and ensure that their patient assistance programs account for different levels of financial need in different therapeutic categories.
[Click to Enlarge]
Figure 1: GoodRx analysis finds a large gap in out-of-pocket (OOP) costs between branded and generic drugs, and the gap is uneven across specialty categories.
HEALTHCARE PROVIDERS STILL UNCERTAIN ABOUT PATIENT OOP COSTS
Even with access to a patient’s insurance information, estimating the cost of prescription drugs remains a challenge for providers. A 2020 survey of 371 providers found that only 21% could accurately estimate OOP drug costs for a hypothetical patient, even with the information in hand. Of course, if you work in healthcare or the insurance industry, you may not be surprised by that.
Another OOP-related survey conducted by GoodRx in 2022 found that 62% of physicians and 53% of all prescribers (MDs, PAs, and NPs) did not discuss medication costs with patients because they were unsure how much the medication would cost their patients.* This survey also found that 64% of physicians said they spoke with their patients about the cost of medications less than 50% of the time. In addition, 54% of physicians said their patients don't ask about the cost of medication, which is why they don't discuss it.
Patients share the responsibility for understanding their OOPs, yet also have a difficult time estimating their prescription drug costs. A 2022 survey from GoodRx found that healthcare costs beyond medication are unclear and confusing for consumers. These include primary care doctor visits, emergency room visits, urgent care visits, medical procedures, and hospital bills.
Insurance cost-sharing is notoriously difficult to understand, and often perplexing even for those who deal with it every day. And it’s not part of the core curriculum during a physician’s many years of training. One result of this complexity is that patients without OOP expectations arrive at the pharmacy only to experience sticker shock which often leads to prescription abandonment. That’s a big problem, because abandonment can endanger patients’ health, make providers’ jobs more difficult, cause unnecessary readmissions to healthcare systems, and cost our economy lost productivity and wages.
IMPROVING OOP COST TRANSPARENCY
To help address the issues of prescription abandonment, lack of information, and limited access to savings offers, GoodRx has developed a range of products and partnerships. One GoodRx partnership enables physicians to see the OOP cost of a medication right in their electronic health record (EHR).
When a patient doesn’t have commercial insurance, the physician is shown the cash price of the medication at pharmacies through the GoodRx network. This enables a discussion about the cost of medication using real-world prices, enabling a better discussion about affordability and cost limits even before the prescription is generated. Additionally, pharma manufacturers partner with GoodRx to elevate their co-pay, cash and other financial assistance programs on the GoodRx platform.
So, instead of guessing about a medication’s cost, providers can use the GoodRx platform to inform their conversations with patients. This creates opportunities for biopharma marketers to message providers through a platform their customers already trust and use frequently. Providers share GoodRx information with patients to raise awareness of affordability solutions such as copay cards offered by drug manufacturers.
PATIENT-PROVIDER COMMUNICATION IS KEY
According to a GoodRx survey, one-third of Americans have trouble paying their medical bills even when they have insurance. Encouraging frank, fact-based discussions about cost between providers and their patients may improve the ability of prescribers to select appropriate medications for their patients that the patient can better afford. When both provider and patient work as a team to gain access to cost-saving opportunities, such as manufacturers’ patient support programs, everyone wins. This teamwork also has an impact on refills, not just new prescriptions. A GoodRx analysis from 2020 suggested that 33.2% of GoodRx fills were newly adherent, meaning they would not have been filled without GoodRx.
Especially in our current economic climate, concerns about out-of-pocket drug costs are top of mind for many patients, especially those taking specialty medications. GoodRx is an important resource for both providers and their patients, connecting them for accurate, transparent, and fact-based conversations about medication options, affordability and pharma access programs. Click here to learn more about the analyses in this article and how GoodRx can help brand teams engage providers in specific specialties.
* Survey conducted by Qualtrics for GoodRx, n=1,098 Physicians, Nurse Practitioners, Physician Assistants, Registered Nurses, and front office staff, conducted between March 1- May 13, 2022. Included 218 physicians, 220 NPs and 218 PAs across clinical settings.
Sponsored guest posts are bylined articles that are screened by Drug Channels to ensure a topical relevance to our exclusive audience. These posts do not necessarily reflect our opinions and should not be considered endorsements. To find out how you can publish a guest post on Drug Channels, please contact Paula Fein (paula@DrugChannels.net).


No comments:
Post a Comment