Click here to see the original post from April 2022.
The highly-consolidated PBM market notched another year of increased concentration.
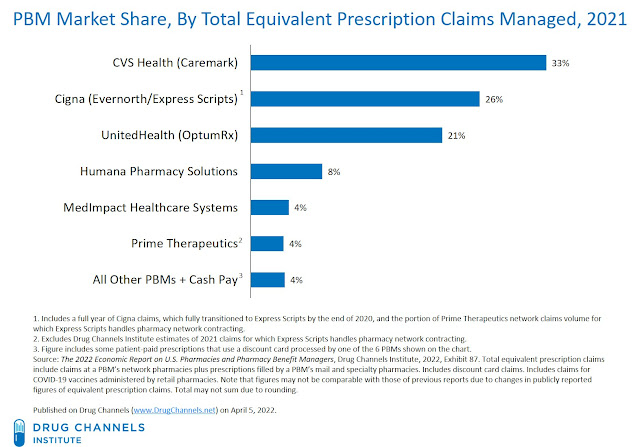
Consider Drug Channels Institute's latest estimates of pharmacy benefit manager (PBM) market share, shown in the chart below. For 2021, we estimate that the three biggest PBMs accounted for 80% of total equivalent prescription claims. Significant business relationships among the largest companies continue to shift market share.
As I explain below, the prospects for market disruption remain low, so the controversial warped incentives of the rebate system will continue to distort the drug channel.
MEET THE MARKET
The market share chart shown below comes from Chapter 5 of our new 2022 Economic Report on U.S. Pharmacies and Pharmacy Benefit Managers. The section numbers below refer to this report.
We estimate that for 2021, 80% of all equivalent prescription claims were processed by three companies: CVS Health (including Caremark and Aetna), the Express Scripts business of Cigna, and the OptumRx business of UnitedHealth Group.
[Click to Enlarge]
When reviewing the figures above, it’s important to consider:
- Vertical consolidation. The concentration shown above reflects significant transactions and business relationships among the largest PBMs that have further concentrated market share. These include CVS Health’s acquisition of Aetna, Cigna’s acquisition of Express Scripts, Anthem’s formation of IngenioRx (and relationship with CVS Health), and the partnership between Express Scripts and Prime Therapeutics. What’s more, all but one of these PBMs—MedImpact—have fully or partially combined into vertically integrated organizations that bring together insurers, PBMs, specialty pharmacies, and healthcare providers.
However, as we discuss in Section 12.3.1. of our new 2022 report, these organizations are still trying to achieve significant vertical synergies. Some have even started to unwind their vertical efforts.
- Claims management. Smaller PBMs often rely on larger PBMs for claims and pharmacy network management. Therefore, the figures for the largest companies include an unknown number of claims from smaller PBMs. Section 5.2.3. highlights more than a dozen of these smaller market participants.
Larger PBMs have also consolidated claims. For example, we estimate that for 2021, Cigna’s Express Scripts business handled pharmacy network contracting for about 40% of Prime Therapeutics’ annualized equivalent claims volume. (See How Cigna’s Growing Pharmacy Platform Expands Its Channel Power.) Cigna includes these claims in its total adjusted prescription claims volume. CVS Health provides various PBM services for Anthem’s IngenioRx business and Centene’s health plans. We believe that CVS Heath’s figures therefore include Anthem and Centene claims.
- Discount cards. Patient-paid prescriptions that use a discount card are not considered cash-pay, because the claims are adjudicated by a PBM. (Here's why.) Examples of discount cards include GoodRx, Blink Health, InsideRx, and Walmart+ Rx for Less. Therefore, a growing share of discount card claims are included within the figures for each PBM. We estimate that discount cards accounted for about 5% of retail prescription activity in 2021. See section 4.3. for more on patient-paid prescriptions.
- Rebate aggregation. The figures above do not correspond to the number of covered lives handled via rebate negotiations. Over the past three years, the largest PBMs have launched new purchasing groups that handle rebate negotiations with manufacturers and provide other services to manufacturers and the groups’ members. To date, these groups are focused on commercial, nongovernment business. Section 5.2.4. profiles the three major PBM-owned purchasing groups: Ascent Health Solutions (Cigna/Evernorth), Emisar Pharma Services (UnitedHealth Group/Optum), and Zinc Health Services (CVS Health).
Amid these changes, PBM compensation models have evolved, due to increased scrutiny by payers, regulators, and politicians. Specialty pharmacy dispensing, participation in the 340B Drug Pricing Program, copay maximizers, and fees from manufacturers have all become crucial to PBMs’ profitability. Meanwhile, the share of PBMs’ gross profits earned from retained rebates and retail network spreads have declined.
Looking ahead, I expect market concentration to remain at a high plateau. The coming years will see some reshuffling of market share among the big three PBMs, as second-tier players outsource more of their PBM business operations to external companies.
However, those readers expecting massive market disruption should lower their expectations. Large employers, health plans, and government payers have shown limited appetite for change and continue to rely on the largest companies for PBM services. I recommend my still-relevant 2017 article: If Employers Are So Unhappy with Their PBMs, Why Can’t They Change the Model?.
By contrast, smaller employers have grown more willing to embrace small players by carving out PBM services from their health plan. (See Section 5.1.2. of our new pharmacy/PBM report.) However, these smaller PBMs often rely on the larger companies for claims processing, rebate aggregation, and pharmacy network management.
So, you should prepare to live with our current PBM market’s golden rule: Whoever had the gold gets to make the rules.

No comments:
Post a Comment